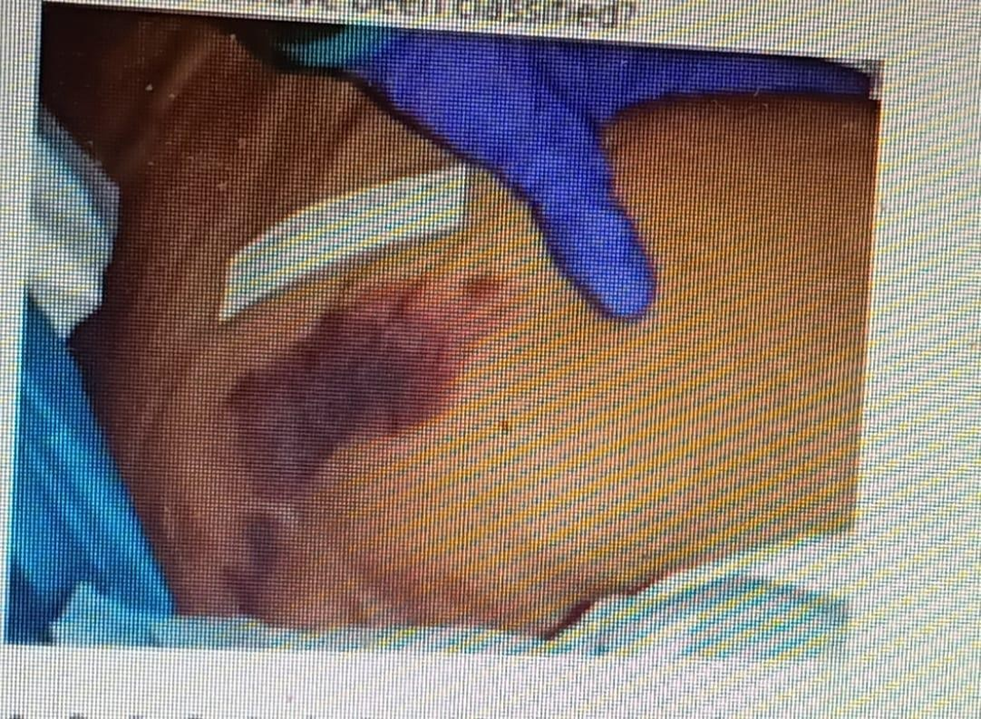
A nurse is completing a chart audit and finds the following wound documented as a Stage I Pressure Ulcer. The nurse recognizes this is incorrect. How should the wound have been classified?
A.
Deep Tissue Injury
B.
Stage III Pressure Ulcer
C.
Unstageable Ulcer
D.
Stage IV Pressure Ulcer
The Correct answer and Explanation is:
The correct answer is A. Deep Tissue Injury.
Explanation:
A Stage I pressure ulcer is characterized by intact skin with non-blanchable redness over a localized area, typically over a bony prominence. It represents the earliest stage of pressure injury development. However, if the documentation indicates a Stage I pressure ulcer, yet the nurse recognizes the assessment does not align with this classification, it’s crucial to consider the other options.
A Deep Tissue Injury (DTI) occurs when there is localized purple or maroon discoloration of intact skin or a blood-filled blister, indicating damage to the underlying soft tissue. This injury can result from pressure or shear and is often difficult to detect in darker skin tones. The initial signs may not be evident, and the skin may appear intact, which can lead to misclassification if not carefully evaluated.
If the wound had progressed to a Stage III or Stage IV pressure ulcer, it would involve full-thickness tissue loss. Stage III involves damage to subcutaneous tissue but does not extend through the fascia, while Stage IV involves extensive destruction, tissue necrosis, or damage to muscle, bone, or supporting structures.
An Unstageable Ulcer is characterized by full-thickness tissue loss where the base of the ulcer cannot be visualized due to slough or eschar. This classification is used when the extent of tissue damage is obscured.
Given the details, if the wound was incorrectly labeled as a Stage I but does not present with non-blanchable redness, and there are signs indicative of a more severe injury, classifying it as a Deep Tissue Injury is appropriate. This classification emphasizes the potential severity of the wound and underscores the importance of ongoing assessment and proper documentation in wound care management. Accurate classification is crucial for appropriate treatment, as it guides interventions to prevent further deterioration and promotes healing.